Bunion Revision Surgery Miami
AVERAGE COST
$8,000 - 12,000
PROCEDURE TIME
20 – 40 Min
BACK TO WORK
2 week
FULL RECOVERY
6 weeks
Book Your Free Consultation
What is bunion revision surgery?
As we already anticipated at the beginning, a bunion revision surgery is one that is applied in cases in which it is considered that a first bunion surgery already performed did not work or did not meet its objectives. This failure of a previous surgery is often referred to as failed bunion surgery. A bunion revision surgery, by definition, is one that is performed after a failed bunion surgery. Whenever an unsuccessful bunion surgery takes place, there remains the option of performing a bunion revision surgery, which exists precisely for that, to correct mistakes made in a previous surgery, or to culminate or perfect the treatment that previous surgeries only started or partially completed.
However, it must be said that bunion revision surgeries are not as frequent as they might appear. This low frequency is due to the fact that the failure rate of normal bunion surgery is very low. The success rate of bunion surgeries is around 98%, which shows the almost resounding effectiveness of the procedure. Of course, bunion revision surgery is needed in a tiny proportion of cases. Even in the remaining 2%, that is, the cases in which normal bunion surgery failed, what will come next will not necessarily be a new surgery. There are non-surgical treatments for revision bunion surgeries.
It should be clarified that what is subjected to revision during bunion revision surgery is not the bunion itself (which will already be more than revised at that point), but the surgery previously performed. Tests are done to find out what went wrong or didn’t work in the previous surgery, and a way is found to make it work and eliminate the patient’s bunions. That is to say, the correct meaning if we group the words in pairs, is that of “revision surgery” and not that of “bunion revision”. A clearer phrase, although it is more extensive and less elegant (that is why it is used less), is that of ” surgery to correct a failed bunion surgery”.
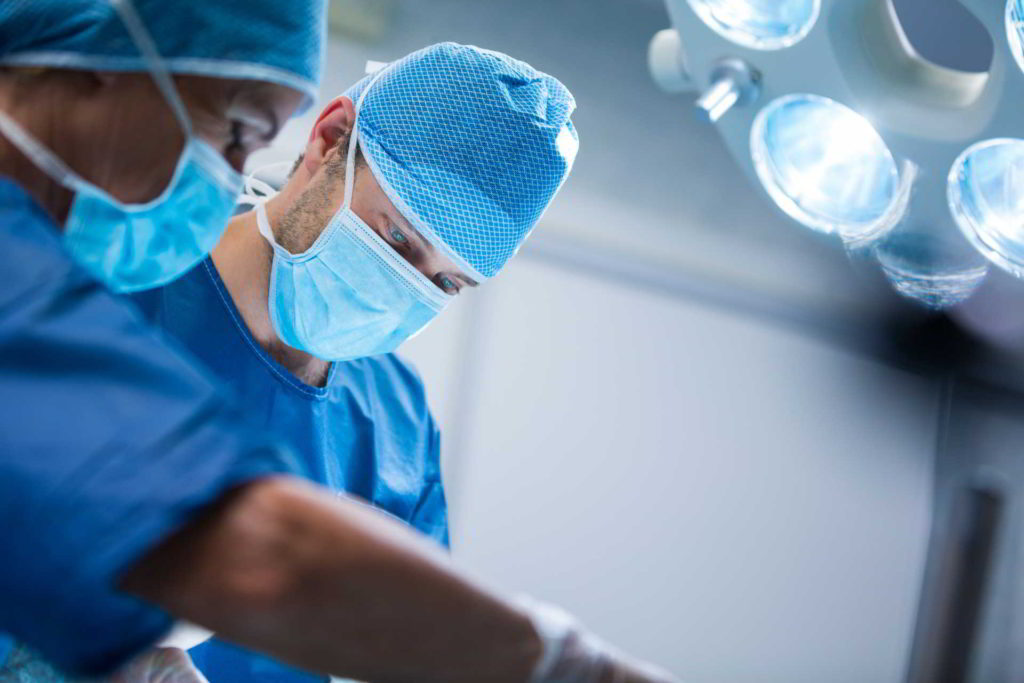
Types of bunion revision surgery
Mild, Moderate, or Severe
One point of view of classification is based on the level of severity of the bunion, and therefore on the degree of complexity of the surgery to correct it in a first or second operation. From this point of view, the types are:
- Mild Bunion: Involving very simple surgery and will almost certainly not require bunion revision surgery.
- Moderate bunion: Involving simple surgery, with minimal possibility of requiring bunion revision surgery.
- Severe bunion: Requiring less straightforward surgery, and having some chance of requiring bunion revision surgery.
As the phrase “bunion revision surgery” is actually generic, any type of bunion surgery is likely to receive bunion revision surgery. Or more clearly stated: any type of bunion that has received surgery (tailor’s bunion, hallux valgus, hallux adductus, hallux extensus, hallux limitus, hallux rigidus), can technically also receive bunion revision surgery if the first surgery did not correct the bunion issue. And we say “technically”, because, as we have already seen, the probability of having a failed bunion surgery is 2% or less.
Possibly the specialist who performs the bunion revision surgery is the same one who did the previous bunion surgery; however, this is not necessarily so. Often, if the first bunion surgery did not work, the patient seeks another specialist to perform the bunion revision surgery.
Osteotomy, Arthrodesis, and Exostectomy
This point of view of classification, which is really the main one, is based on the technique used to correct, reposition and realign the toe with the bunion, as well as to eliminate the bump that deforms the toe. The surgeon, after studying the case, will previously decide which of the following three techniques to apply during surgery. In the case of bunion revision surgery, the specialist must decide if he will apply the same technique as in the previous surgery, or if he will opt for a new one, with the aim of achieving greater effectiveness. The three techniques are as follows:
- Osteotomy: This is the most widely used procedure. Through the previously made incision, the surgeon corrects and aligns the bones, and fixes their position using small screws or pins that will later be removed.
- Arthrodesis: This consists of extracting the affected part of the joint and repositioning it in a corrected position through the support of screws. It is applied in very severe cases, in which bunions are combined with arthritis.
- Exostectomy: It is the least used of the three techniques since it is reserved for cases of really mild or undeveloped bunions. It is also called “bunion shaving”, because it consists of scraping the joint that does not present too pronounced deformity. This technique can be combined with an osteotomy.
Surgical or Conservative
Another point of view to classify the possible revision surgery after bunion surgery is based on the method to be followed for the correction. From this point of view, the method to correct the errors or insufficiencies of a previous bunion surgery can be surgical or non-surgical (in the latter case it is called the “conservative” method). The decision to apply non-surgical methods to correct bunion surgery errors will depend on the simplicity or severity of the case, as well as the patient’s health conditions and habits.
In the event that the specialist from other clinics decides to perform bunion revision surgery, it remains to choose whether it will be conventional bunion surgery or a minimally invasive bunion surgery. However, in the case of Luxe Foot Surgery, it will be a minimally invasive bunion surgery ( Minimally Invasive Bunion Surgery In Miami ). What is minimally invasive bunion surgery? This is one of the most frequent questions that patients ask us. To answer it, we must start from the fact that traditional bunion surgeries involve larger incisions, and therefore, more pain and longer recovery periods.
Instead, minimally invasive bunion surgery overcomes all of that. In this case, the entire procedure is performed through a very small incision at the base of the big toe. Thanks to this, pain is minimized and the surgery is treated as an outpatient operation, so the patient returns home the same day, without admission to the clinic, and recovery occurs in a much shorter time. You can learn more about this topic on our YouTube channel.

What are the goals of bunion revision surgery?
Basically, the objectives of bunion revision surgery consist of correcting or completing errors or insufficiencies of any previous bunion surgery. But in addition to correcting the insufficiencies of some previous surgery, the primary objectives of any bunion surgery remain: to eliminate the pain produced by the bunion, to correct the musculoskeletal deformity of the foot, to restore the aesthetic appearance of the foot as close as possible to the natural one, and return to the foot its functions when walking, standing or performing various daily activities.
Cost of bunion revision surgery in Miami
The cost range for bunion surgery across the United States is between $7,500 and $13,500, with an average of $8,500. But, as is always the case, in the state of Florida, and especially in Miami, medical costs may be below the US average. At Luxe Foot Surgery we offer an average price of $8,000 for bunion surgery, and we have in-house payment plans that provide extra facilities. The surgery takes no more than 20 to 40 minutes, so it is considered to be walk in, and avoids many collateral expenses.
Something to keep in mind is that at Luxe Foot Surgery we treat bunions with minimally invasive surgery. This has great economic benefits, which are included even if they are not noted in the price. The patient can return to work in just 2 weeks, which guarantees that the economic impact of not working is minimal. To this is added that complete recovery is obtained in only 6 weeks. These return to work and complete recovery times are exceptionally short when compared to those of conventional bunion surgery.
When is it considered that bunion surgery failed and should a review be done?
Bunion surgery is considered to have failed when it did not meet the goal of removing the bunion and restoring functionality to the foot. Failure is also considered to be the fact that, although the bunion symptoms disappeared immediately after surgery, they returned shortly after, according to what is called “bunion return”. This does not necessarily indicate surgeon error, but simply things that can happen.
Bunion surgery also fails when, instead of eliminating or improving the condition of the bunion, the condition of the foot worsens due to what is called anatomical overcorrection. In these cases, the pain caused by the bunions may not only not have disappeared but may even have increased due to the surgery.
The same can happen with the flexibility of the foot. The patient may experience excessive stiffness in the toe, and may even feel immobile. Another indicator that bunion revision surgery is needed is that previous surgery failed to visually correct the deformity of the toe, or even deformed it further or in a new way. In the worst case, the surgery may have added a new type of bunion or foot deformity.
Quite often, bunion revision surgery is performed by a different surgeon than the one who performed the first surgery. This may be due to the fact that the patient, noticing that the first operation failed, seeks a doctor who will guarantee that the second operation will not fail. It is important that, in the case of bunion revision surgery, the patient has a specialist who has the experience, this is even better if he has extensive experience. Almost always this new surgeon will have to correct delicate mistakes made by the previous surgeon.
Who is a good candidate for bunion revision surgery?
A good candidate for bunion revision surgery is anyone for whom a first bunion surgery has not solved the problem, has not solved it at all or has made it worse. It is also important to determine, through a study, if what did not work from the first surgery was the procedure itself. The patient is no longer a good candidate for a bunion revision surgery if what caused the first surgery to not work was some health condition, chronic illness, or even bad habits that the patient is not willing to give up.
For example, if the bones and tissues did not heal after bunion surgery because the person first developed diabetes, or if the bunions returned after surgery because the person did not stop wearing the wrong shoes or plan to stop wearing them, possibly the surgeon himself would not recommend performing the bunion revision surgery, because the probability of success would be very low.

Importance of slow recovery to increase the chance of success
Recovery after conventional bunion surgery is quite long and can take anywhere from 6 months to a year. The same is not true of the minimally invasive bunion surgery that we offer at Luxe Foot Surgery , which is accomplished in 1 and a half months. However, the recovery time after a bunion revision surgery is not the same. In these cases, a little more time may be required to achieve a full recovery. As the amount of recovery time in this type of surgery is based on the status of the previous surgery, it is recommended that the specialist be the one to communicate to the patient how long they should rest and when they will be fully recovered.
It is convenient to plan the recovery time. Modifications will have to be made to the structure, dynamics, and rhythm of the home. You have to take enough time off work. Some housework will fall on other people, and if the bedroom is on an upper floor, it is convenient to bring the bed to the lower floor, so that the patient does not have to force his foot up the stairs.
What are the risks of bunion revision surgery?
All surgery involves some risks, which may or may not occur. Among the normal risks of bone surgeries are:
- Adverse reactions to anesthesia (even if the patient’s body had not reacted like this on other occasions).
- Excessive bleeding, blood clots, and thrombus dangers.
- Infections (although this is minimized thanks to minimally invasive surgery).
- The possible (although unlikely) damage to the blood vessels and nerves near the bunion.
- Failure of the bone to heal, blood circulation problems, and prolonged swelling of the foot.
But surgeries on surgeries carry a bit more risk, especially if the bunion revision surgery is being performed by a different surgeon than the one who performed the original surgery. So is bunion revision surgery riskier than regular bunion surgery? The answer is yes. Bunion revision surgery is considered by many doctors to be not only riskier, but even much riskier than regular bunion surgery.
One of the risks involved is the excessive correction of the musculoskeletal structure related to the toe with the bunion. While undercorrection is uncomfortable, so is overcorrection, which will cause severe stiffness or even immobility in the toe In a small percentage of cases, bunion revision surgery can lead to a condition in which the big toe is shorter than normal or extremely deviated, or even points toward the opposite foot.
Causes of bunion surgery failure that lead to revision surgery
Some causes of bunion surgery failure are due to errors or lack of experience of the surgeon or medical staff, but others are due to the patient’s own failure. In addition to these two reasons, there are causes that are not due to the surgeon or the patient but simply to normal risks that are implicit in any surgery. The causes of bunion surgery failure can be:
- That the doctor has made mistakes in a previous surgery. For example, if the bone cut is made at the wrong angle, as a consequence setting or healing may occur poorly or not at all.
- Sometimes the errors are due to the surgeon’s lack of experience, but sometimes they are due to insufficient study of the case before surgery. There is no identical bunion surgery for all cases. Each case is relatively different, so bunion surgery requires choosing the appropriate surgical technique for the case, and also personalizing and adapting it to the patient.
- If it is the patient requiring a third bunion revision surgery after two failed surgeries, the surgeon for the second operation may not have been experienced enough to correct the mistakes of the first.
- That certain health conditions of the patient (such as diabetes, cardiovascular disorders, allergies to metals, etc.) have hindered or prevented bone or wound healing.
- That the patient, for hereditary or genetic reasons, has anatomical shapes that force him to maintain wrong postures when supporting his foot or walking, despite the corrections received through bunion surgery.
- That the patient has not followed to the letter the advice and prescriptions that the surgeon gave him at the end of the first bunion surgery. For example, if the whole body was supported excessively on the foot which was operated on, if he walked with inappropriate footwear, or if he did not rest enough or did not rest long enough.
Outcomes of bunion revision surgery measured by the AOFAS scale
The AOFAS scale (acronym for the American Orthopedic Foot And Ankle Society) is called a standardized instrument used to measure the clinical status of the ankle and hindfoot, from three points of view: pain, functionality, and alignment. Both objective and subjective information are used for this measurement. The score goes from 0 to 100, but only healthy joints receive 100 points (getting more than 90 points after surgery is a great achievement). Doctors often evaluate the results of bunion revision surgery using the AOFAS scale. Let’s look at some examples.
One study demonstrated a mean improvement of 59 to 90 points on the AOFAS scale, in a bunion revision surgery based on the replacement of the crescent osteotomy technique (performed in the first surgery, which had caused a recurrence of hallux valgus deformity) for a chevron osteotomy. This bunion revision surgery performed on a 39-year-old woman managed to almost completely correct the bunion after a 3-month recovery, without causing recurrences.
Coetzee JC, Resig SG, Kuskowski M., et al., members of the Department of Orthopedic Surgery, the University of Minnesota (in a study entitled « The Lapidus procedure as salvage after failed surgical treatment of hallux valgus: a prospective cohort study » ) , recommend applying the Lapidus type arthrodesis in bunion revision surgeries after failed hallux valgus surgeries. With this procedure, the AOFAS score can increase from 45 to 90 points, and the mean intermetatarsal angle can decrease from 18.0° to 8.6°.
Frequently asked questions
Here you have the frequently asked questions section that we promised you at the beginning. We have briefly answered the main questions of patients regarding bunion revision surgery. Always remember that if your question is not reflected or answered in this section or in other parts of our website, you can contact us and schedule an appointment to bring your case to a specialist.
As with normal bunion surgery, bunion revision surgery can be performed at virtually any age. It is clear that bunions are more frequent in people over 45 years of age, and that is why bunion surgery and bunion revision are more frequent at these ages. But that does not mean that bunion surgery or bunion revision surgery cannot be performed at other ages if necessary.
In fact, bunions even occur in children, although more for genetic and hereditary reasons than for reasons of musculoskeletal wear, poor posture, excessive use of inappropriate footwear, etc. When it comes to younger people, with the body in full development and growth, attempts are made by all means to eliminate bunions using conservative and non-surgical techniques such as changes in posture, the use of appropriate footwear or orthopedic devices such as splints, orthotics, wraps, ridges, tubes, etc.
Bunion revision surgery is not necessarily recommended for all patients whose first bunion surgery has failed. However, second bunion surgery is recommended if after the first surgery if:
- You experience severe pain in the ftoe or in the area.
- You feel that the toe which was operated upon has unusual stiffness.
- Perceive post-surgical arthritis, bone necrosis, or any disorder that compromises the normal function of the foot.
However, the decision to perform bunion revision surgery is primarily made by the surgeon, after the patient communicates the symptoms and after the relevant tests are performed.
Bunions affect women more than men, and older women more than girls. This is a popularly known fact and even statistically proven. In boys and girls, bunions are specifically a problem of genetic inheritance, not because the bunions themselves are inherited. What is inherited is the anatomy of the foot, the way of walking, the posture when standing or sitting, etc. But why do bunions affect women more than men? This is a very frequently asked question.
The answer is that women probably, for reasons of beauty and much more frequently than men, wear inadequate and uncomfortable shoes, with high and thin heels, with a thin toe and are tight fitting, which keeps the toes compressed and the foot in poor condition, the wrong posture, and sustained bone and muscle contraction. When this type of shoe (which pushes the big toe in and puts excessive pressure on the first metatarsal) becomes common, bunions can develop.
According to the medical literature and the criteria of some older specialists, there are more than 100 techniques from which bunion surgery can be applied. However, the vast majority of these techniques are no longer put into practice, and mainly those that we saw above are used (osteotomy, arthrodesis, and exostectomy).
Many of the previously used techniques are due to the different types of bunions and the surgical ways of approaching their treatment, necessarily different from each other because it is not the same, for example, operating a hallux valgus or bunion in the big toe than a tailor’s bunion or little toe bunion, located on the diametrically opposite part of the foot.
In the case of traditional bunion surgery, full successful recovery takes between 6 months (to return to normal physical activities) and one year (to return to the practice of sports and other strenuous physical activities). However, in the case of a minimally invasive bunion surgery like the one we make available to you at Luxe Foot Surgery, the return to normal work activities is achieved in an astonishingly short time: barely 2 weeks, counted from the day of surgery. And the total recovery, with us, is also very short: in 6 weeks, that is, in approximately 1 month and a half, the patient will be fully recovered.
If the patient underwent bunion surgery, and subsequently required bunion revision surgery, it is possible that this was due to bad habits that did they not break after the surgeries, which caused the emergence and re-emergence from bunions. Except in the case of genetic problems, if the patient follows exactly what the doctor recommends and prescribes, and if he abandons the habits that caused the bunion, the reappearance of bunions does not have to become recurring.
However, if the patient does not comply with what is recommended by the specialist and does not give up bad footwear habits, foot posture, or gait, the bunions could reappear chronically.
A completely logical question is whether bunions can return after bunion surgery. Treatment as drastic as surgery is supposed to eliminate bunions forever. The answer is that it doesn’t necessarily eliminate them, or at least not in all cases. If the patient does his or her best, follows all of the podiatrist’s advice, and breaks the habits that led to the bunion, the chance of the bunion recurring and the need for bunion revision surgery is minimal. Some things that the patient can do to avoid bunion recurrences are:
- Avoid the use or excessive use of high-heeled, pointed-toe, tight-fitting or smaller-size footwear than the one that naturally corresponds to your foot.
- Maintain use of orthopedic support devices and accessories if recommended by the physician.
- Consume the drugs that the doctor has prescribed and follow the prescribed method.
- Eliminate foot calluses. If the calluses are recurring, eliminate the action that causes them.
Non-surgical methods to treat bunions are based, in addition to changes in habits and foot postures when walking, on the use of oral or injectable drugs, and on the use of orthopedic accessories that help distribute the stress evenly. This helps spread the body weight between your feet and eliminates stress on your toes. Some of these accessories may be in the form of insoles, socks, or foot or toe wraps, while others are purely plastic, silicone, or metal combination devices such as straightening ridges, splints, and orthotics.
The effectiveness of these non-surgical or conservative methods to treat bunions depends on three strong factors:
- The mildness or severity of the bunion condition: If the bunion is only mildly developed, or even in its early stages, there is a high chance that non-surgical methods will work. In contrast, if the bunion is at an advanced level of development, non-surgical methods are less likely to work.
- The dedication that the patient puts into the treatment: The degree of dedication that the person has when putting into practice and following up on the treatment is of great importance. Non-surgical treatments, although they avoid having to go into an operating room, are not even remotely comfortable. If the patient adheres to the letter of what is recommended by the doctor or maintains the correct use of the devices, however uncomfortable they may be, the chances are high that the bunion will be reduced or eliminated. But if the patient does not persevere and has random behavior regarding the prescription, the chance that non-surgical treatment will work is very low.
- The age of the patient and the cause of the bunion: In all this, the age of the patient plays an important role. If it is a very young patient or even a child, the cause of the bunion will probably be genetic or hereditary, and since it is a developing body, there are possibly very few bad habits to correct. But if the patient is an adult or older adult, the bunions may be due to a lifetime of bad habits and musculoskeletal wear, and it will be less easy to correct the bunions non-surgically.
A very frequent question that patients ask us refers to when they can put pressure back on their feet after bunion revision surgery. Another very frequent question related to the previous one is: How soon can the patient walk again after bunion revision surgery? The answers to these questions are quite positive, which is another of the advantages of the minimally invasive surgery that we offer you at Luxe Foot Surgery. As it is an outpatient and minimal access surgery, the patient will remain resting in the postoperative care unit for 1 to 2 hours after surgery. After this, you can return home.
This means that the patient will receive the instructions in the practice itself when he is still in the clinic and is preparing to go home. At this point, the medical staff will recommend that you put pressure on your feet as little as possible, but you don’t need to avoid it altogether. The important thing, for now, is to prevent the weight of the body from falling on the operated foot, until 2 weeks have passed and the foot can be supported normally.
The doctor will provide the patient with a special type of shoe made to measure. Wearing such special footwear is an essential part of the recovery process. After 1 month or a month and a half, the patient will have the foot fully recovered and will be able to walk normally.
With respect to whether or not insurance covers bunion revision surgeries, as is always the case, the determining factor is whether it is a medical or aesthetic condition. If the previous bunion surgery caused effects that cause the patient pain or interfere with their normal life, this is considered a medical problem and not merely an aesthetic one, for which reason the insurance will generally cover the bunion revision surgery (within the terms of the contract that the patient has obtained, that is, according to the percentages and deductibles of the policy).
On the other hand, if the effects left by the first bunion surgery belong to the area of the merely aesthetic, this will not be considered a medical problem and, in general, health insurance will not cover bunion revision surgery, or at all. the case will not cover most of the total cost.
Latest Articles

What to Expect After Haglund’s Deformity Surgery
When Haglund’s deformity proves to be resistant to all non-surgical remedies, such as changing footwear, anti-inflammatory drugs, and physiotherapy, surgical
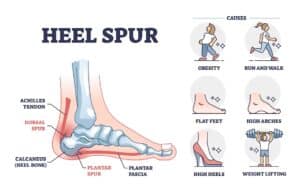
Dorsal Heel Spur Surgery – Procedure, Recovery, and What to Expect
Dorsal heel spur surgery is a procedure that alleviates irritating symptoms caused by heel spurs that develop on the back
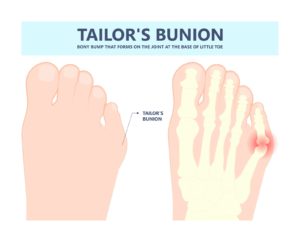
Bunion on the Little Toe: Causes, Symptoms, and Treatment Options
Many individuals struggle with a bunion on the little toe – this condition can cause unpleasant symptoms and interfere with

How to Treat the Bursitis of a Bunion
When there is a bunion, one of the common complications that can occur is bursitis. This condition is an inflammation
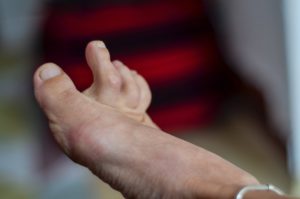
Failed Hammertoe Surgery: Causes, Complications, and Solutions
No matter how experienced a doctor is or how routine the procedure, every surgery poses a certain amount of risk

Floppy Toe After Hammertoe Surgery: Understanding the Phenomenon
Even though hammertoe surgery is a routine, minimally invasive procedure, it still carries a certain amount of risk. One of

Toe Shortening Surgery in Atlanta: A Comprehensive Guide
Foot health is always overlooked until a person starts having difficulties while walking and standing for longer periods of time.

Understanding the Stages of Healing for a Plantar Wart: A Comprehensive Guide
Skin conditions on your feet can be difficult to fully get rid of, which is why it’s so important to

Plantar Wart vs. Callus: How to Differentiate Between the Two
A lot of different skin conditions present themselves in a similar fashion on our feet – rough bumps or patches

Plantar Wart vs. Corn: Understanding the Differences
It’s well-known that plantar warts and foot corns aren’t the same thing – but they still often get confused with

Bone Spur or Bunion: Understanding the Difference
Bone spurs or bunions are different orthopedic issues that can create foot pain and discomfort. Even though they have distinct

Bunion Recovery Week-By-Week Process
Bunion surgery is a highly successful procedure, and most patients recover from it very well and in a short amount