Treatment for Athlete's foot
At Luxe Foot Surgery, we are dedicated to providing highly effective treatment for athlete’s foot in Miami. Our center offers a range of options to meet the needs of our patients. We have a team of specialists who are extensively trained and experienced in treating athlete’s foot. From the moment you step through our doors, you will receive compassionate, ethical, and professional care. Our goal is to ensure your comfort and satisfaction throughout your visit, and our facilities are designed to provide a pleasant experience.
- Updated on: January 16, 2024
AVERAGE COST
$1,500
PROCEDURE TIME
20 – 40 Min
BACK TO WORK
1 week
FULL RECOVERY
2 weeks
Book Your Free Consultation
What is Athlete's Foot?
Athlete’s foot is the most common skin infection caused by a group of fungi that thrive on and infect the feet. It derives its name from the fact that athletes, due to their profession and the type of footwear they wear, are more prone to this type of infection.
The fungi that cause athlete’s foot are known as dermatophytes. Dermatophytes feed on keratin, a type of protein found in the skin cells that line the internal and external surfaces of the body. Some of the most common fungal species that cause athlete’s foot include:
- Trichophyton rubrum
- Trichophyton interdigitale
- Epidermophyton floccosum
This fungal infection is characterized by a rash or redness accompanied by itching, burning, and even cracking of the skin. It can appear on one or both feet at the same time.
Other Names for Athlete's Foot
Athlete’s Foot is known by various other names, such as tinea pedis, a term derived from Latin which translates to “ringworm of the foot” in English. It is also referred to as “foot ringworm” or simply “fungal infection of the feet.”
Furthermore, some may simply refer to it as a fungal foot infection or fungal dermatitis affecting the feet. Regardless of the name used, the symptoms and treatment options for Athlete’s Foot remain consistent. It is important to promptly address the infection to prevent its spread and alleviate discomfort.
Global Statistics on Athlete's Foot
Athlete’s Foot is a widespread condition that can affect individuals across the globe, regardless of their geographical location. Studies suggest that the prevalence of Athlete’s Foot is on the rise, making it one of the most common skin infections seen by dermatologists.
Statistics reveal that approximately 15% of the global population experiences fungal foot infections or Athlete’s Foot. It is estimated that around 70% of the population will either have or have had tinea pedis at some point in their lives. In other words, 7 to 8 out of every 10 individuals may be affected by Athlete’s Foot. Clinical research also indicates that 20% of individuals may be asymptomatic carriers of contagious tinea infections.
To combat the global prevalence of Athlete’s Foot, it is crucial to raise awareness about prevention measures, proper foot hygiene, and early treatment. By adopting preventive strategies and seeking timely medical attention, individuals can reduce the risk of contracting and spreading this common fungal infection.

How much does athlete's foot treatment cost in Miami?
How is athlete's foot diagnosed?
The diagnosis of athlete’s foot typically relies on a clinical evaluation of symptoms and the appearance of the affected skin. The dermatologist will conduct a thorough visual examination of the feet and may ask questions about the experienced symptoms, the duration of the condition, and any triggering factors. However, to confirm the diagnosis and determine the type of infectious agent present, additional tests may be performed.
One common test is the collection of skin samples for laboratory analysis. These samples can be obtained by scraping the skin with a sterile blade or by using adhesive tape to collect surface cells from the skin. These samples will be examined under a microscope to detect the presence of fungi or other microorganisms causing the infection. Therefore, it is important to consult a dermatologist for an accurate diagnosis and a proper treatment plan.
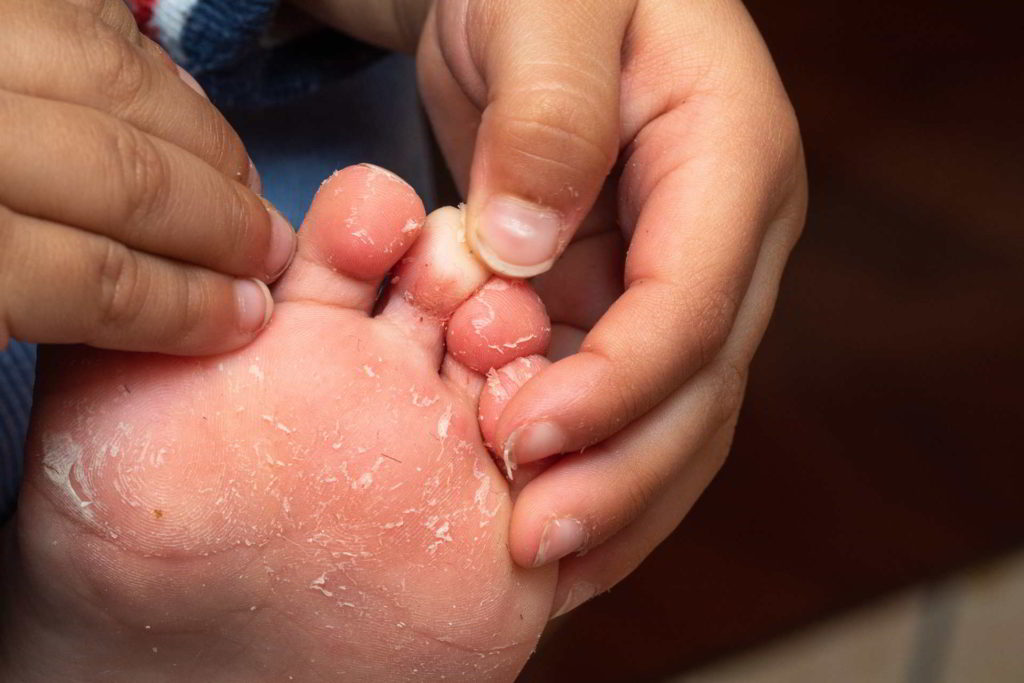
What does athlete's foot look like?
Athlete’s foot can alter the appearance of the skin on the feet in various ways. Depending on the type of tinea pedis infection, the skin may appear red, purplish, grayish, or whitish. The fungus can affect the spaces between the toes, spread across the entire sole of the foot, or even extend to the top of the foot. Another common area of infection is the edges of the feet and the heels, which is known as “moccasin-type athlete’s foot.” The skin may be irritated, blistered, cracked, or scaly.
In addition to the visual changes in the skin, athlete’s foot can also cause discomfort and symptoms such as itching, burning, and a stinging sensation. The affected skin may feel dry and rough to the touch. If left untreated, the infection can spread and worsen, causing further damage to the skin and potentially leading to secondary bacterial infections.
Four Types of Athlete's Foot
Athlete’s foot can be classified into different types based on the appearance of the skin and the affected area of the foot. Each type may present different symptoms and require specific treatment. Here are the four main types of athlete’s foot:
Interdigital Athlete’s Foot (Tinea Pedis): This is the most common type of athlete’s foot, and it affects the skin between the toes. It typically occurs between the fourth and fifth toes, but can also affect the membranes of other toes. The affected skin may change color, become whitish, and exhibit peeling, irritation, scaling, and even cracks. Foul odor is also a common symptom. Athlete’s foot weakens the skin, making it vulnerable to bacterial infections that can further deteriorate the skin.
Moccasin-Type Athlete’s Foot (Tinea Pedis): Also known as dermatophytosis, this type can affect the sole of the foot, as well as the edges and heel. It gets its name from the appearance it gives to the edges of the foot, resembling a moccasin-style shoe. This infection can initially cause foot pain. Over time, the sole of the foot and the edges of the heel become thickened and hardened. This can lead to cracks that, if left untreated, may deepen and cause bleeding. Moccasin-type athlete’s foot also causes skin scaling. In severe cases, it can spread to the toenails, causing them to thicken, crumble, and eventually fall off.
Vesicular Athlete’s Foot (Tinea Pedis): This type of athlete’s foot typically appears on the sole of the foot, particularly the inner or arch area, but can also occur anywhere on the foot. It is also known as inflammatory athlete’s foot. Vesicular athlete’s foot is less common than the interdigital or moccasin types. It is characterized by the sudden outbreak of fluid-filled bumps or blisters known as vesicles. These blisters can be painful, cause skin irritation, and may rupture, leading to discomfort and a higher risk of bacterial infection. Vesicular athlete’s foot can be particularly odorous.
Ulcerative Athlete’s Foot (Tinea Pedis): Ulcerative athlete’s foot is the least common type. It usually occurs between the toes, similar to interdigital athlete’s foot. However, the ulcerative type causes deeper, moist lesions. It is characterized by open sores or ulcers, some of which may develop on the sole of the foot. Ulcerative athlete’s foot requires prompt medical attention due to the increased risk of infection and complications.
Identifying the specific type of athlete’s foot is important for determining the most appropriate treatment approach. If you suspect you have athlete’s foot, it is advisable to consult a healthcare professional for an accurate diagnosis and personalized treatment plan.
Symptoms Indicating the Need for Athlete's Foot Treatment
While there are different types of athlete’s foot, the symptoms tend to be fairly common across the various forms. If you experience any of these symptoms, it is likely that you require treatment for athlete’s foot, and you should seek the assistance of a dermatologist. The most common symptoms associated with different types of athlete’s foot include:
- Cracked and scaly skin in certain areas of the feet.
- Persistent itching and burning sensations in the feet.
- Presence of a rash or skin eruption.
- Burning and itching sensations between the toes and other areas of the foot.
- Development of small, fluid-filled blisters beneath the skin.
- Appearance of white, red, or discolored patches on the skin of the feet.
- Noticeable foot odor, even when the feet are clean.
- Swollen and tender areas when putting weight on the foot.
- Hardening of the edges of the foot.
- Areas of the skin that may ooze or become moist, in more severe cases.
- Raw, exposed skin in certain areas.
If you are experiencing any of these symptoms, it is important to seek medical attention for a proper diagnosis and to discuss suitable treatment options. Prompt treatment can help alleviate discomfort, prevent the infection from spreading, and promote faster healing.
Causes of Athlete's Foot
Athlete’s foot is a fairly common fungal infection that is actually not difficult to contract. Even a slight contact with an infected person can be the cause of its appearance. There are many ways in which athlete’s foot can occur, which is why it is important to take precautions to prevent it. The most common causes of athlete’s foot include:
- Coming into contact with the skin of a person who is infected with athlete’s foot.
- Walking barefoot in public places where there is moisture, such as swimming pools, showers, saunas, gyms, etc.
- Frequent use of closed shoes with little or no breathability, leading to foot sweating.
- Engaging in sports with inappropriate footwear.
- Having frequently or prolonged periods of wet feet.
- Being male. Males are more prone to athlete’s foot infection than females.
- Having small wounds on the nails or feet, which increases the chances of contracting dermatophytes.
- Older adults are at higher risk of contracting athlete’s foot.
- Sharing intimate accessories with infected individuals, such as towels, flip-flops, shoes, socks, etc.
- Reusing damp or sweaty socks from the previous day.
- Not allowing shoes to air out after use.
- Always wearing the same footwear without rotating them to allow for proper drying.
- Not applying antifungal products to shoes, such as powders, sprays, etc.
By being aware of these causes and taking preventive measures, such as practicing good foot hygiene, wearing breathable footwear, and avoiding direct contact with infected individuals, it is possible to reduce the risk of developing athlete’s foot.
Who is More Susceptible to Athlete's Foot?
As mentioned earlier, the term “athlete’s foot” originated from the fact that athletes or sports enthusiasts have historically had a higher incidence of this type of infection. Therefore, athletes, who have even given the condition its name, are one of the groups at higher risk of developing athlete’s foot. This is due to the prolonged exposure of their feet to a moist and warm environment, as a result of their intense training and the type of footwear commonly used in sports. Statistics show that about 70% of people who experience athlete’s foot during the summer are athletes or engage in sports activities.
In general, certain factors can increase an individual’s susceptibility to developing athlete’s foot. These include:
- Athletes and Sports Enthusiasts: People who participate in sports or engage in activities that involve prolonged foot sweating and use communal areas like locker rooms or showers are more prone to athlete’s foot.
- Individuals with Sweaty Feet: Excessive sweating of the feet creates a moist environment that promotes fungal growth, increasing the risk of athlete’s foot.
- People with Weakened Immune Systems: Individuals with compromised immune systems, such as those with diabetes, HIV/AIDS, or undergoing immunosuppressive therapy, have a higher susceptibility to fungal infections like athlete’s foot.
- Individuals with Poor Foot Hygiene: Poor foot hygiene, such as not regularly washing and drying the feet thoroughly, can contribute to the development of athlete’s foot.
- Wearing Tight or Non-Breathable Footwear: Wearing shoes and socks that do not allow proper ventilation and trap moisture can create an ideal environment for fungal growth.
- Walking Barefoot in Public Places: Walking barefoot in public areas like pools, gyms, or communal showers increases the risk of coming into contact with the fungi that cause athlete’s foot.
- Sharing Personal Items: Sharing items such as towels, shoes, or socks with an infected individual can facilitate the spread of the fungi responsible for athlete’s foot.
While anyone can develop athlete’s foot, taking preventive measures such as practicing good foot hygiene, wearing breathable footwear, and avoiding prolonged exposure to moist environments can help reduce the risk of infection.
Risk Factors for Developing Athlete's Foot
Athlete’s foot, a common fungal infection, can affect anyone, but certain factors can increase the risk of developing the condition. By understanding these risk factors, individuals can take proactive measures to prevent and manage athlete’s foot. Here are the key risk factors to be aware of:
Warm and Humid Environments: Athlete’s foot thrives in warm and moist conditions, making individuals living in tropical or humid climates more susceptible to the infection.
Excessive Foot Sweating: People who experience excessive sweating of the feet, a condition known as hyperhidrosis, create a favorable environment for the growth of fungi.
Poor Foot Hygiene: Neglecting proper foot hygiene, such as not washing and thoroughly drying the feet regularly, increases the risk of developing athlete’s foot.
Tight or Non-Breathable Footwear: Wearing shoes and socks that are tight-fitting or made of non-breathable materials can trap moisture, creating an ideal environment for fungal growth.
Walking Barefoot in Public Areas: Walking barefoot in communal areas like locker rooms, public showers, and swimming pool areas exposes the feet to the fungi that cause athlete’s foot.
Sharing Contaminated Items: Sharing towels, socks, shoes, or other items with someone who has athlete’s foot can lead to the spread of the infection.
Weakened Immune System: Individuals with weakened immune systems, such as those with certain medical conditions or taking immunosuppressive medications, have a higher risk of developing athlete’s foot.
Existing Medical Conditions: Certain conditions, including diabetes and peripheral artery disease, can increase the likelihood of developing athlete’s foot due to compromised blood circulation and immune function.
Engaging in Water-Related Activities: Participating in activities that involve prolonged foot exposure to water, such as swimming or using hot tubs, without proper foot protection can increase the risk of contracting athlete’s foot.
Prolonged Moisture on the Feet: Wearing wet shoes or socks for extended periods, such as during sweaty workouts or rainy weather, can create an environment conducive to fungal growth.
By being aware of these risk factors, individuals can take preventive measures, such as practicing good foot hygiene, wearing breathable footwear, and avoiding walking barefoot in public areas, to reduce the likelihood of developing athlete’s foot.

When Should You Consult a Specialist for Athlete's Foot?
While many cases of athlete’s foot can be prevented and treated with good hygiene practices and over-the-counter antifungal products, there are instances where professional medical intervention is necessary. Here are some signs that indicate it’s time to consult a specialist for athlete’s foot:
Persistent Symptoms: If the symptoms of athlete’s foot, such as itching, redness, and discomfort, persist despite practicing proper foot hygiene and using over-the-counter treatments, it is advisable to seek medical attention.
Worsening Condition: If the symptoms worsen over time or spread to other areas of the feet, it may indicate a more severe infection that requires professional treatment.
Compromised Immune System: Individuals with weakened immune systems, such as those with diabetes or HIV/AIDS, should consult a specialist promptly, as they are at higher risk of developing complications from athlete’s foot.
Suspected Secondary Infections: If you notice signs of a secondary bacterial infection, such as increased pain, pus, or spreading redness, it is crucial to see a specialist for appropriate diagnosis and treatment.
Recurrent Infections: If you have a history of recurring athlete’s foot infections, it is recommended to consult a specialist who can assess underlying factors and provide long-term management strategies.
At Luxe Foot Surgery, our experienced specialists offer effective treatments for athlete’s foot. If you experience persistent or worsening symptoms, we recommend scheduling a free consultation to receive a proper diagnosis and personalized treatment plan.
What is the Specialist Called Who Prescribes Treatment for Athlete's Foot?
The medical professional who specializes in foot and ankle disorders is called a podiatrist. In some countries, the terms podiatrist and podologist are used interchangeably. However, in the United States, a podiatrist refers specifically to a physician specializing in foot care, while a podologist is typically associated with beauty treatments for the feet. The podiatrist is primarily responsible for providing treatment to eliminate athlete’s foot.
Since athlete’s foot is a widespread infection, it falls within the realm of infectious diseases. Therefore, an infectious disease specialist, also known as an infectiologist, may also be involved in the treatment and management of fungal infections of the feet. In exceptional cases, athlete’s foot may be associated with immune system disorders or can lead to them. In such instances, in addition to the podiatrist and infectiologist, the patient may need to consult with an immunologist.
Regardless of the specialist involved, seeking professional medical advice and treatment is crucial to effectively manage and eradicate athlete’s foot.

What questions should I ask the specialist during the consultation for the treatment of athlete's foot?
Many patients simply receive treatment passively, without probing into more details with the specialist. The truth is that if the patient is more aware of what they have and how the disorder behaves, they are likely to be able to contribute more to their recovery. From hygiene measures during treatment to prophylaxis to prevent athlete’s foot from returning once eliminated, all of this works better if the patient understands what they are doing. Not to mention that during an interview of this type, the patient can provide even more detailed information to the doctor.
What type of athlete’s foot do I have and what are its characteristics? Understanding the specific type of fungal infection in my feet will help me better recognize its appearance and maintain optimal hygiene measures.
Besides medication, what additional measures should I take during the treatment? The specialist will provide specific advice based on the individual case. For example, depending on the type and severity of the infection, the treatment duration may vary from 3 to 6 weeks or longer if extended post-treatment safety measures are necessary to prevent reinfection.
Do I need to make any dietary changes during this treatment? While it is rare, some patients may need to modify their normal diet due to antifungal treatment. For instance, individuals with compromised immune systems or certain chronic conditions may require medication that interacts with antifungal drugs. The extent of dietary adjustments will be determined by the doctor.
What is the likelihood of reinfection? The answer to this question depends on the patient’s occupation or activities. It is important for the doctor to be aware of the patient’s profession. If the individual is an athlete, a frequent swimmer, or regularly uses public showers, skis, skates, or rubber boots, the doctor may provide specific measures to prevent reinfection.
Remember, by actively engaging with the specialist and asking these questions, you can enhance your understanding of the condition, optimize your treatment, and take preventive measures to reduce the risk of recurrence.

Types of Medical Treatments for Athlete's Foot
Medical treatments for athlete’s foot typically revolve around antifungal medications. These products have shown high effectiveness, although they do not guarantee the prevention of reinfection. Some are available over-the-counter, while others require a prescription from a specialist. Generally, before applying a topical antifungal product such as ointments, gels, creams, lotions, powders, sprays, or aerosols, it is important to thoroughly wash the feet.
Cases of mild to moderate athlete’s foot are often treated with topical medications, which are commonly available without a prescription. These treatments can be divided into two main groups: allylamines (including terbinafine and naftifine) and azoles (including bifonazole, clotrimazole, miconazole, and oxiconazole). Advanced cases or those that do not respond to topical treatments may require oral medications. Finally, severe cases are often treated with a combination of topical medications and oral pills. Let’s take a look at some specific antifungal products used in the treatment of athlete’s foot:
- Clotrimazole (Lotrisone)
- Econazole (Ecoza, Spectazole)
- Ciclopirox (Loprox, Penlac)
- Terbinafine (Lamisil)
- Itraconazole (Sporanox, Tolsura)
In addition to the mentioned pre-treatment foot washing, medical treatments for athlete’s foot include certain precautionary measures we have discussed and will continue to explore in this article. These measures include avoiding excessive use of closed-toe shoes that cause foot sweating (especially for individuals prone to excessive sweating), refraining from using towels, bedding, clothes, shoes, or socks of infected individuals, not reusing unwashed socks, and thoroughly disinfecting footwear that has come into contact with fungal-infected feet, among others.
Frequently asked questions about athlete's foot treatment from Luxe Foot Surgery patients
Our patients at Luxe Foot Surgery often ask some frequent questions about athlete’s foot treatment. Below, we will answer some of these questions, because we know it may be the doubt of other people. If you have another question to ask us and it does not appear here, we invite you to call us directly. Also, if required, you can schedule a first free appointment with the specialist. Remember that at Luxe Foot Surgery, we have financing plans. It will be a pleasure to assist you!
Generally, athlete’s foot is not a serious condition, although this does not mean that it should not be monitored. The fungal infection can spread to other parts of the body, such as nails or groin; but this happens infrequently. The biggest danger is that athlete’s foot can cause other skin infections, such as cellulitis, as bacteria can penetrate the skin through the lesions and worsen the situation. But these things usually do not happen when there is treatment for athlete’s foot.
The prognosis for patients is good, as long as they receive good treatment for athlete’s foot. To achieve a quick recovery, patients should follow all care instructions that the specialist will give, and thus avoid relapses of contagion during the treatment for athlete’s foot. If patients comply with these hygiene measures and are disciplined with the treatment, the fungus will eventually be eliminated.
Do not use other people’s shoes or socks or allow others to use yours, because there is a high probability that you will transmit the fungus to them. Also, do not use old shoes or other people’s shoes that are suspected of having athlete’s foot or have had it. This fungus is notably persistent, even though the shoes have been unused for a long time.
This is especially true for cases of closed sports shoes or water boots, but precautions should also be taken with ski shoes or skating in public rental places. If you cannot avoid using shoes of these types, it is best to disinfect them before using them. For this, you can use antifungal sprays or powders.
If you are receiving treatment to eradicate athlete’s foot fungus, or if you have already received it, disinfect all the shoes you normally use. This will prevent you from reinfecting yourself, or the fungus from passing from one shoe to another. It is also advisable to disinfect and rid towels, sheets, and all bed linen of pathogens. You will probably be able to achieve this if you use special fabric disinfection products.
There are many measures that can be taken to prevent the spread of athlete’s foot, either to avoid spreading it to other people or to other areas of the body. Among the most useful measures to avoid contracting athlete’s foot are:
- Wash your feet and the skin between your toes with special antifungal soap.
- Dry your feet well after bathing, or at the end of a sporting event.
- Use talc or antifungal powder on your feet to absorb moisture.
- One way to prevent the fungus from spreading to the groin is to put on socks before underwear.
- Use shoes that allow good foot perspiration and do not accumulate sweat.
- Give shoes at least 24 hours of rest after using them, so that sweat does not accumulate due to continuous use.
- Avoid using rubber shoes or synthetic materials as much as possible.
- Regularly clean shoes with disinfectant sprays or wipes.
- Wear socks that are made of natural materials and that absorb sweat, such as cotton and wool.
- Do not walk barefoot in public places like gyms, saunas, pools, public showers, etc., or wash your feet very well after doing so.
- Wash intimate clothing, bed linen, as well as socks, with hot water. This helps to eliminate microorganisms that may be lodged in the fibers.
Home remedies can be effective, and that’s why doctors sometimes recommend them. However, in cases of advanced athlete’s foot, or if the home treatment has no effect after 10 days or at most 2 weeks, we recommend at least using over-the-counter antifungal drugs. Using a mildly effective home remedy can cause a delay that allows the infection to progress, and then the specialist will have to prescribe relatively invasive drugs, such as oral antifungal medications. However, we reiterate, home treatments for athlete’s foot can be effective in many cases of mild or non-advanced infection, and side effects are usually rare. Any unexpected reaction should stop the use of the product. Here are some of these treatments.
- Baking soda: It’s a very common household product and is always acquired at very low prices. It has antifungal properties. Its use is simple: add half a cup of baking soda to a bucket of water or equivalent container. Soak your feet in this solution for 20 minutes up to twice a day. At the end, dry your feet but do not rinse them, to let the baking soda continue to act.
- Cornmeal Corn: can contain a natural fungus, which while harmless to the body, kills the fungus that causes athlete’s foot. To make it: Mix one cup of cornmeal and two liters of water in a container in which you can soak your feet. Allow the cornmeal to rest in the water for 1 hour. Finally, soak your feet in that solution for about 1 hour.
- White vinegar or apple: cider vinegar Vinegar is a product with antifungal properties. Although it does not seem capable of eliminating athlete’s foot in homemade preparations, it does have the property of relieving the infection and calming the itching and pruritus that the fungus produces between the toes. To use it, add a couple of tablespoons of vinegar to between 750 ml and 1 L of water, and soak your feet in this solution for 20 minutes up to twice a day. At the end, dry your feet, but do not rinse them.
- Mouthwash: Usually, mouthwash is capable of eliminating bacteria and germs that enter the mouth. For the same reason, it may be capable of eliminating bacteria and germs from the feet. The antiseptic ingredients work to keep bacteria and fungi away, as long as the infection is very mild and there is no better solution at hand. You can mix the mouthwash with white vinegar in equal parts, and put the mixture on the area of fungi for half an hour. This can be repeated twice a day.
- Hair dryer + Talc: Fungi need a humid environment to develop. If they don’t have it, they don’t develop or spread even though they are present. That’s why removing moisture from the feet and between the toes helps prevent the fungus from spreading or worsening. A good method to thoroughly dry the toes and the area between the toes is to use a common hair dryer, either after bathing or at any time. Once the feet are well dried, talc can be applied to them.
- Tea tree oil Tea: tree oil has many applications, including as an antifungal. It can be applied as a balm to infected fingers, being careful to wash hands very well at the end.
- Lavender oil: Lavender oil has antiseptic properties and also helps prevent skin irritations. It can be applied to the affected areas of the foot, left to act for 10 to 20 minutes, and finally rinsed off. This can be repeated several times a day. In addition to athlete’s foot, it can be used to eliminate toenail fungus.
- Garlic or onion Garlic, among its many qualities, includes antifungal properties that can help eliminate foot fungi. An important component of garlic in this regard is allicin. It can be used to eliminate both athlete’s foot and toenail fungus. You should mix crushed garlic (or pre-made garlic oil) with white vinegar. Apply this mixture to the infected area and then cover it with a bandage and keep it on for a few hours. This should be repeated daily until the fungus disappears. The onion also has antifungal properties that can help eliminate athlete’s foot. Its preparation and application are very similar to those of garlic.
- Hydrogen peroxide: with iodine The first thing to say is that this is one of the home treatments that should be practiced with caution. It is common for peroxide and iodine to be present in homes, as they are used, among other things, to disinfect skin cuts or other types of wounds. Their action eliminates germs from the skin, but sometimes they are a bit excessive. In some places they have been contraindicated. However, it is known that peroxide in combination with iodine is capable of eliminating various types of fungi. Optimal results are obtained if they are used together, not separately. To apply this home remedy, mix iodine and hydrogen peroxide in a bucket with water, and then soak your feet. You can also use a cotton ball to apply the preparation directly to the affected areas. IMPORTANT: Do not use iodine on the skin without first diluting it, because it can damage it. Also, peroxide can cause a lot of itching if the skin is cut or irritated; it can also discolor hair and clothing, so it must be handled with care.
- Socks of special fabrics: Not using traditional cotton socks, but other types of socks whose fabric absorbs the moisture of the skin, can be considered a treatment in cases of very mild athlete’s foot infections. This, in addition to helping keep feet dry, helps stop the advancement of the infection in very early stages. Among the types of socks that can help keep feet dry during the day and therefore have positive effects on athlete’s foot, we have wool, bamboo, and so-called smart socks. Of course, even with special fabric socks, hygiene must be maintained.
Yes, athlete’s foot is a fungus that is easily contagious. It can be transmitted from one person to another, or to different areas of the same body. For example, if your feet are infected with the fungus and you scratch a lot with your hands, the infection can also spread to your hands. Therefore, precautions and hygienic measures should be taken to prevent the spread of athlete’s foot. On surfaces in places where humidity is constant (such as swimming pools, showers, etc.), the fungus that causes athlete’s foot can survive for months.
The answer to this question depends on the severity or degree of athlete’s foot progression. Normally, infections from this type of fungus can range from mild to severe. Although in all cases a positive outcome can be expected, only the milder infections are eliminated within a period of 2 to 3 weeks. Topical medications or oral antifungal drugs should be maintained for the prescribed period, with the aim of minimizing relapses or recurrences.
Sometimes athlete’s foot fungal infections are not easy to eradicate, even if strong antifungal or antimicrobial drugs are being used, not just simple home remedies. In these cases, treatment must last longer, up to approximately 6 weeks. It is necessary to continue with the treatment for a longer period, even if the fungus has apparently disappeared. This long-term treatment with antifungal medications, even beyond the time when the fungi have disappeared from sight, is necessary to prevent athlete’s foot infections from returning in the most severe cases.
To reduce the treatment time to the shortest possible period, prophylactic measures must be taken, such as keeping feet clean and dry, wearing socks to prevent the fungus from being absorbed into shoes, avoiding keeping feet in humid environments for too long, avoiding contact with places where you suspect the infection is present, among others.
Yes, athlete’s foot is a fungus that is easily contagious. It can be transmitted from one person to another, or to different areas of the same body. For example, if your feet are infected with the fungus and you scratch a lot with your hands, the infection can also spread to your hands. Therefore, precautions and hygienic measures should be taken to prevent the spread of athlete’s foot. On surfaces in places where humidity is constant (such as swimming pools, showers, etc.), the fungus that causes athlete’s foot can survive for months.
This type of fungus spreads easily. If you don’t undergo treatment for athlete’s foot, it can extend to the sole of the foot and develop into a moccasin-type infection. Severe cases of athlete’s foot can cause skin cracks, inflammation, fluid-filled blisters, and even ulcers.
Without treatment, athlete’s foot will continue to spread, making the person an infectious agent in their environment. Precautions must be taken at home and in places the person frequents to avoid infecting others. The symptoms can also worsen if the fungus is not stopped with treatment, leading to strong foot odor and increasingly unbearable itching. Another consequence of not treating athlete’s foot is that it can spread to other areas of the body, such as:
- Nails: Untreated athlete’s foot can also infect the toenails. Once the fungus settles between the hard layer of the nail and the skin, it becomes much more difficult to eliminate. Nail infections caused by athlete’s foot often become resistant to many treatments.
- Hands: The fungal infection from athlete’s foot can also spread to the hands. This happens when patients have the habit of scratching their feet and not washing their hands afterward. The fungus can also transfer to the hands through towels when the same towel is used for infected feet and the rest of the body.
- Groin: Dermatophytes can also settle in the groin area, causing jock itch. This usually occurs when the same towel is used to dry both the feet and the rest of the body. It’s important to note that this can also happen if the groin area is not properly dried after bathing, whether at home or in pools, beaches, etc.
Mild to moderate cases of athlete’s foot can often be treated effectively with specific home remedies and improved personal hygiene. If the foot does not exhibit symptoms such as bleeding, fluid or pus discharge, nail involvement, and if the skin condition shows signs of improvement and responds well to treatment, the situation should not worsen. Over-the-counter antifungal medications are commonly used for treating athlete’s foot. However, it is important to note that there are still risks associated with self-treatment.
If you have any doubts or concerns, it is always recommended to seek the opinion of a healthcare professional. Prescription medications should never be consumed without the proper guidance and prescription from a specialist. Oral medications, in particular, can have potent active ingredients that may lead to side effects and drug interactions. For example, oral terbinafine may cause gastrointestinal disorders, as well as temporary loss of taste and smell. Some studies have shown a very low risk of severe liver damage with the use of these oral antifungal medications. Therefore, individuals with liver disease are only prescribed these medications if absolutely necessary.
Additionally, other antifungal drugs may interact with active ingredients in medications the person is taking for other reasons. Due to these potential risks, it is crucial that only a specialist prescribes and authorizes the use of such medications. Avoid self-medication and prioritize your safety.
Yes, it is possible to become reinfected after successfully treating athlete’s foot. Similar to other fungal infections, such as toenail fungus, the infection can often recur, especially if the patient did not seek professional treatment and attempted to eliminate the fungus with home remedies or over-the-counter medications. If the foot fungus persists, it is necessary to consult a specialist for appropriate treatment.
It is also important to reinforce the hygiene measures we mentioned earlier, such as thoroughly washing the feet, avoiding reusing worn socks, minimizing the use of closed-toe shoes, and so on. Additionally, on days when you anticipate wearing shoes for an extended period, using antifungal powders can help keep your feet dry and prevent the proliferation of fungi despite wearing shoes.
Latest Articles
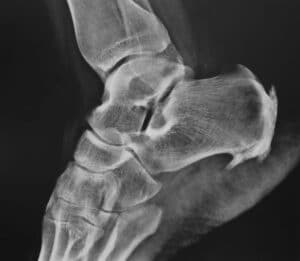
The Breakdown of Haglund’s Deformity Surgery Cost
Haglund’s deformity is a bony protrusion on the back of the heel. This podiatric condition is a result of calcaneus
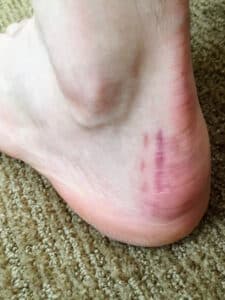
What to Expect – Haglund’s Deformity Surgery Scar
Haglund’s deformity or syndrome is a protrusion on the back of the heel caused by an enlargement of the calcaneal
How Long Does Haglund’s Deformity Surgery Tak
Haglund’s deformity, also known as Mulholland deformity, is a bone and soft tissue abnormality on a person’s heel. It causes
Managing Pain After Haglund’s Deformity Surgery – What to Expect and Tips for Relief
Make the recovery phase after Haglund’s deformity surgery a breeze. Learn tips and tricks for managing pain after Haglund’s deformity

What to Expect After Haglund’s Deformity Surgery
When Haglund’s deformity proves to be resistant to all non-surgical remedies, such as changing footwear, anti-inflammatory drugs, and physiotherapy, surgical

Can Haglund’s Deformity Recur After Surgery? Understanding the Possibilities
When it comes to some of the most stubborn health issues, foot conditions are at the top of the list.
Haglund’s Deformity Post Surgery: A Comprehensive Guide
Each surgical procedure has a unique recovery period, no matter how minimally invasive it is. There will be certain things
What Are the Main Haglund’s Deformity Surgery Risks? An In-Depth Overview
As with any other medical procedure, Haglund’s deformity surgery comes with its own set of risks and potential complications. Before

Returning to Running After Haglund’s Deformity Surgery – A Guided Journal
When can you return to running after Haglund’s deformity surgery? Physical therapy and a smooth recovery process impact how soon
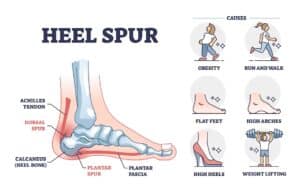
Dorsal Heel Spur Surgery – Procedure, Recovery, and What to Expect
Dorsal heel spur surgery is a procedure that alleviates irritating symptoms caused by heel spurs that develop on the back

Understanding the Costs of Laser Corn Removal
Alleviating discomfort and nagging pain caused by corns on the patient’s feet has never been easier to do. Removing painful

Minimally Invasive Hammertoe Surgery Cost – An Informative Guide
Do you need pain relief from a bent toe joint? Fortunately for many patients, there is a minimally invasive surgery