Haglund Deformity Surgery
Welcome to Luxe Foot Surgery, your go-to clinic for Haglund Deformity Surgery in Miami. Our specialization lies in managing intricate foot conditions, including Haglund’s Deformity. With a dedicated team of experts, we focus on providing personalized care that restores your comfort and mobility. In this article, we will concisely cover all aspects of Haglund Deformity Surgery in Miami, including the cost, frequently asked questions, and much more. Let us accompany you on your journey to improved foot health.
AVERAGE COST
$16,000
PROCEDURE TIME
30 – 40 Min
BACK TO WORK
2 - 3 week
FULL RECOVERY
3 - 6 months
Book Your Free Consultation
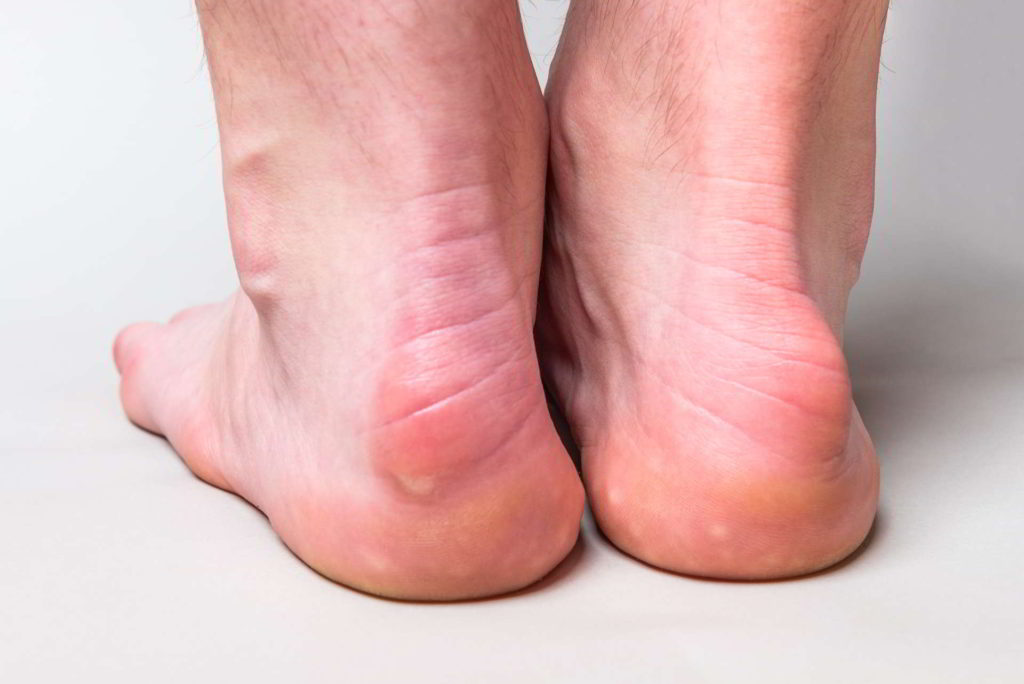
Understanding Haglund Syndrome and Deformity: What You Need to Know
Haglund syndrome or deformity is characterized by a protrusion on the back of the heel. This protrusion is caused by excessive enlargement of the bone and appears right where the Achilles tendon is located. Sometimes, this deformity does not cause pain, but in other cases it does. When Haglund syndrome occurs, the Achilles tendon is usually irritated or calcified. Inflammation can worsen due to the pressure exerted by shoes on the area where the tendon attaches to the bone, causing the bags to become inflamed. Haglund’s deformity is more common in patients with a hollow or cavus foot.
Haglund’s syndrome or deformity can combine to give a triad of conditions:
- Insertional Achilles Tendinopathy
- Inflammation between the Achilles tendon and the heel bone, which is known as Retrocalcaneal Bursitis.
- A Bone Prominence that appears on the top of the heel bone, which is the Haglund deformity itself, is a common symptom of Haglund syndrome or deformity.
Not everyone with Haglund syndrome or deformity needs surgery. In fact, surgery is only recommended as a last resort. The goal of surgery is to remove the prominence of the heel bone and alleviate pain symptoms. It may also involve the removal or repair of a part of the Achilles tendon.
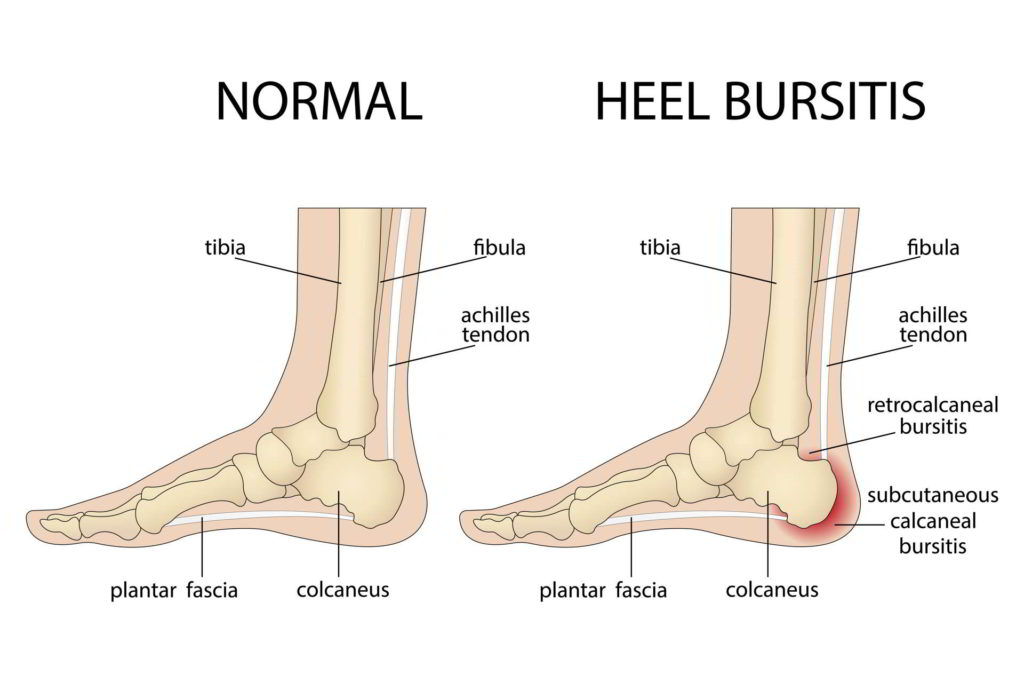
Anatomy of Haglund Deformity
The heel bone, also known as the calcaneus in anatomy, is the largest bone in the foot. The Achilles tendon, which is large in size, attaches to the back of the calcaneus bone. Between the bone and the Achilles tendon, there is a lubricated tissue sack known as a bursa. The bursa allows the Achilles tendon to easily slide against the bone during movements of the foot.
When Haglund deformity occurs, a protrusion or crest on the calcaneus bone is observed on the back of the heel. The tissues associated with this area, such as the bursa, can also become inflamed on the protrusion and create a callus. This callus can grow and thicken, especially with the use of tight shoes. The Achilles tendon can also become inflamed.
Causes of Haglund's deformity
Hollow Foot
The deformity of the hollow foot is usually one of the main causes of Haglund’s syndrome. The hollow foot consists of the longitudinal arch of the foot being more pronounced or higher than normal. This causes, when walking, only the forefoot and heel to touch the ground, which determines that the heel bone or heel bone is in an altered position. For this reason, the back of the heel moves backward, and the Haglund deformity appears.
Hereditary and Biomechanical
- Genetic information plays an important role in the Haglund deformity. People most likely to develop this disorder are those who have family members who also suffer from the deformity. The following characteristics can be inherited:
Type of foot structure in supination, leading to walking on the outside of the heel. - Heel bone with a prominence or crest on the back that rubs against the Achilles tendon.
- Tight Achilles tendon.
Training Tension
Some athletes or people who engage in intense training may start to suffer from the Haglund deformity. Runners are especially advised not to exercise on hard or uniform terrain, because this causes special tension on the heel. Running uphill should also be avoided. The ideal is to run on professional tracks designed specifically for this activity.
Use Tight Shoes
Wearing very tight shoes frequently is another cause of Haglund’s deformity. Shoes with tight toes should also be avoided. Even shoes that are poorly fitted in which the foot can slide should be avoided, as this significantly increases pressure on the heel. It is recommended, as a preventive measure, to use open or soft material shoes. The goal is to generate the least amount of pressure on the heel bone.
Obesity and overweight
Patients with obesity and overweight can develop Haglund’s deformity when they stand for long periods of time every day. The body weight rests on the foot, which generates a strong constant pressure. The extra weight causes the deformity to not be able to be corrected normally through conservative treatments, because the cause, which is the weight, does not change. The most recommendable is that the patients start losing weight so that the high basic load that is maintaining or worsening the disorder can be relieved.
Due to its ultra-minimally invasive nature, it allows for a reduction in surgical and post-surgical complications. From the first day after surgery, patients can walk using crutches. Even after the operation, they can perform active, dorsal, and plantar flexion of the ankle. From the third and seventh days, full support of the foot is allowed, depending on the patient’s condition.

Symptoms of Haglund's deformity
Many patients who come to the clinic for the diagnosis of Haglund’s syndrome report the following symptoms:
- Pain and inflammation in the heel and ankle area
- Swelling and redness in the heel
- Stiffness and difficulty moving the foot
- Limited range of motion in the foot and ankle
- Tenderness to touch on the heel
- Visible bump or protrusion on the back of the heel
- Irritation or rubbing of the Achilles tendon caused by the bony protrusion
- Difficulty wearing certain types of shoes
- Limping or altered gait while walking or running
It is important to note that these symptoms may vary in severity and that not all individuals with Haglund’s syndrome will experience all of these symptoms. It is important to consult a healthcare professional for proper diagnosis and treatment.
How is surgery for Haglund's deformity performed?
It is important to note that not all patients with Haglund’s deformity require surgery. In fact, many patients can improve with conservative treatment methods such as physical therapy, the use of orthotic devices, and shoe modifications. A study conducted at a clinic in Texas found that 89% of patients were able to improve without the need for surgery.
Surgery for Haglund’s deformity is typically only considered for patients who have not seen improvement with non-surgical methods. The surgery is usually performed as an outpatient procedure, with the patient able to go home the same day. The procedure involves making an incision on the back of the heel, next to the Achilles tendon, to remove the bony protrusion causing irritation. In some cases, the surgery may also involve removing inflamed tissue from the retrocalcaneal bursa or releasing or repairing the Achilles tendon if it has become tight or inflamed.
Recovery time after surgery can take several weeks, and physical therapy may be required to help restore strength and range of motion to the foot and ankle. It’s important to consult with a healthcare professional to determine the most appropriate treatment options for Haglund’s deformity.
Types of surgery for Haglund's deformity
There are several types of surgery for Haglund’s deformity. Choosing one method or another will depend on the conditions in which each patient is found. Surgery for Haglund’s deformity is specifically known as calcaneoplasty. Calcaneoplasty is the surgical technique that remodels the posterior edge of the calcaneus bone, with the aim of reducing friction on the Achilles tendon. Let’s take a look at some of the most commonly used techniques.
Open calcaneoplasty
Open surgery with the medial and lateral approach is performed on the heel. The incision is 4-5 cm. Bursectomy is performed as well as resection of the heel crest, and subsequently the debridement or repair of the damage to the tendon.
Endoscopic or minimally invasive calcaneoplasty
The same steps are taken as for the surgery we saw in the previous step, but with less aggression. Only two small puncture incisions are made. The small openings are made on each side of the Achilles tendon, just before its insertion into the heel bone. Minimally invasive calcaneoplasty promotes a much faster recovery for the patient.
Zadek surgery or heel bone correction
This type of surgery for Haglund’s deformity is usually done open, although some surgeons perform it with endoscopy. It is a special technique in which an osteotomy of the heel is performed in cases where the bone is severely enlarged, when the Achilles tendon enthesis is chronically irritated, or when there is a comorbidity in the tendons and ligaments. The surgery consists of removing a wedge of the heel bone, which permanently corrects the deformity.
Ultrasound-guided or non-open calcaneoplasty
It is the least invasive option of all, thanks to the fact that it is performed using local anesthesia. The incision is only 1 mm. Everything is done with direct control of the main structures, and with care not to damage the sural nerve with the beam. The approach and pain is minimal, and therefore the recovery of patients is much faster.
Due to its ultra-minimally invasive nature, it allows for a reduction in surgical and post-surgical complications. From the first day after surgery, patients can walk using crutches. Even after the operation, they can perform active, dorsal, and plantar flexion of the ankle. From the third and seventh days, full support of the foot is allowed, depending on the patient’s condition.
What type of anesthesia is used in surgery for Haglund's deformity?
General anesthesia can be used, or a nerve block can be performed from the knee to numb the entire leg. Generally, the patient can choose the type of anesthesia they prefer. People who are more nervous are recommended general or twilight anesthesia to avoid hearing or seeing the procedure. At the end of the operation, a further dose of anesthesia can be injected to reduce postoperative pain. Additionally, the doctor may indicate a pain management plan after the operation if they feel it is necessary.
How long does it take to correct Haglund's deformity through surgery?
Haglund’s deformity surgery typically takes around 30 minutes to complete. However, if the patient’s conditions are a bit more complex, it may take longer. This time should also include the time the patient needs to stay at the clinic. For example, it is recommended to arrive at the clinic an hour or two before the surgery, in order to complete any necessary paperwork before entering the operating room.
Additionally, patients may need to stay for another hour or two after the surgery to wait for the anesthesia to wear off. After this, they can typically return home the same day as it is an outpatient procedure. Overnight stays are very rare.

What is the cost of Haglund's deformity surgery in Miami?
The cost of Haglund’s Deformity Surgery in Miami typically falls between $16,000 and $18,000. This estimate encompasses a variety of components such as the surgeon’s fees, anesthesia, facility charges, and post-operative care. However, the specific costs can differ based on the individual’s case complexity and the healthcare provider selected. This investment in your health offers significant benefits such as pain relief and improved mobility, making it a worthwhile consideration.
Always discuss with your healthcare provider or insurance company about any potential financial aid or payment plans available.
Benefits of Haglund's deformity surgery
After surgery for Haglund’s deformity, patients experience a wide range of benefits that improve their quality of life. These benefits become fully apparent as they go through the recovery stages. Among these benefits are:
- The protrusion of the heel bone or calcaneus is eliminated.
- Pain disappears after a reasonable recovery period.
- Patients can return to any type of activity.
- It has a low level of risks.
- It is an outpatient procedure, which means that patients can return home the same day.
- It can be performed with minimally invasive techniques.
- Complete mobility of the foot is restored.
- It improves the aesthetics and posture of the foot.
- It restores the health of the Achilles tendon and the bursa.
It’s worth noting that these benefits may vary based on the specific condition and treatment of each individual patient.
Risks of surgery for Haglund's deformity
No surgical procedure is without risks, and surgery for Haglund’s deformity is no exception. Statistics show that a high percentage (between 70-80% of patients) who undergo surgery for Haglund’s deformity are successful. This evidence shows that the balance tilts more towards the benefits than towards the risks. However, it is important to inform our patients about the potential risks of this procedure. Let’s take a look:
Infection
The incidence of infections after surgery for Haglund’s deformity is relatively low. It is estimated that around 5% of patients experience it. Most infections can be resolved with a course of antibiotics. In cases where a deeper infection develops, the solution will be to perform another operation. However, in general, if the initial and post-operative care instructions are followed, the risk decreases. Another detail to keep in mind is that one must see the doctor immediately if there is suspicion of infection.
It’s important to note that the risk of infection can be influenced by a variety of factors, including the patient’s overall health, the type of surgery, and the patient’s ability to follow postoperative instructions properly. Your surgeon will provide you with detailed instructions to follow before and after the surgery to minimize the risk of infection.
Nerve Damage
During the operation, there is always a risk of injuring or stretching the surrounding nerves. This can cause numbness or even a feeling of weakness. Generally, the symptoms disappear over time, but they can persist for quite some time.
It’s important to note that nerve damage is a potential complication of any surgery, including Haglund’s deformity surgery. Your surgeon will take great care to minimize the risk of nerve damage during the procedure, but it is still a possibility. If you experience any numbness or weakness after the surgery, it is important to inform your surgeon right away. In most cases, the symptoms will resolve over time, but in some cases, further treatment may be necessary.
Delayed Wound Healing
Medical literature reflects that approximately 3% of patients experience some type of wound complication after surgery for Haglund’s deformity. This is a relatively low level, however, it can still occur because the blood supply to the back of the ankle is limited. If the bone or wound takes a long time to heal, another plastic surgery may be required. An important recommendation is not to smoke during this period, as nicotine affects the healing process.
Swelling
Swelling appears almost immediately after surgery for Haglund’s deformity. The Achilles tendon can become swollen as part of the healing process that the body undergoes as a response to the surgery. The swelling will completely disappear within 12 months. During this time, the operated foot tendon will appear more bulky than the non-operated one.
Achilles Tendon Rupture
It is very rare for the Achilles tendon to tear after surgery for Haglund’s deformity. In these cases, an additional surgery is required, and the recovery period will be longer. In situations like these, patients are strongly urged to strictly follow the postoperative care instructions.
It’s important to note that the risk of Achilles tendon tear is low, but it can happen in rare cases. It’s important to follow the postoperative instructions provided by your surgeon to minimize the risk of complications and to ensure a successful recovery. Additionally, your surgeon will monitor your recovery closely and will provide you with any additional instructions or treatment as needed.
Pain Syndrome
In some patients, chronic regional pain syndrome (CRPS) may occur after surgery for Haglund’s deformity. The foot becomes painful, swollen, and sensitive recurrently. In these cases, patients should see a pain management specialist.

Who are candidates for Haglund's deformity surgery?
Candidates for surgery for Haglund’s deformity are those who have already tried various conservative methods and have not seen improvements. The doctor will evaluate the best option for the patient based on their health conditions, age, and the characteristics of the deformity. There are no restrictions or limitations for those who need this surgery. However, it is important to inform the doctor of any health conditions to minimize risks. Only a few people with specific health complications will not be able to have the surgery.
Stages of recovery after surgery for Haglund's deformity
The recovery time for a surgery for Haglund’s deformity has different stages, which are organized by weeks and months. Each stage follows certain guidelines that patients must follow, as the success of the operation largely depends on these.
First week of recovery
Patients will leave the hospital with a cast below the knee, so that the foot does not bear the weight of the body. This is when the most pain will be felt, but the surgeon will have guided a pain management plan. Swelling is another condition that must be avoided with anti-inflammatory drugs. The medications should be taken with meals or after meals. The foot should be kept elevated, above hip level, for as long as possible, to avoid the formation of bruises.
Circulation should also be cared for by doing this exercise: drawing circles in the air by moving the toes. The patient should only stand up to go to the bathroom, and when doing so, they should use crutches correctly. In some cases, the use of ice bags may be recommended to reduce swelling and pain. It is advisable to drink a lot of water to avoid blood clots. During bathing, the cast should be well covered to avoid getting wet.
Second week of recovery
At this stage, the pain should decrease significantly. Ten days after surgery, the stitches are removed, and physical therapy exercises can begin. Light support of the foot with crutches can also be started. By the end of the second week, one of the exercises can be riding a stationary bike and leaving one of the crutches. It is the stage in which patients can start showering normally. All this is done if the doctor believes that the patient is already fit.
From the fourth to the sixth week of recovery
Between the fourth and sixth weeks of recovery, muscle strengthening exercises are continued. These include exercises for proprioception, flexibility, stationary bike and elliptical machine. After six weeks, patients can begin to jog gently.
From the third to the sixth month of recovery
At this stage, a final review of the surgery is done with the specialist. At this point, inflammation should be minimal and the patient should be able to perform most of their regular activities. This period should see the return of normal walking, and even running may be possible. Competitive sports may also be resumed, but not at a high-performance level.
Twelve months after surgery
At this stage, both swelling and residual discomfort should significantly improve and almost disappear between 12 and 18 months. By this time, patients should be enjoying all the benefits of surgery for Haglund’s deformity.

Tips for recovery from Haglund's deformity surgery
The recovery period is a key factor for the success of Haglund’s deformity surgery. Some tips to follow include:
- Keeping the cast dry and clean until it is removed by the doctor.
- Keeping the foot elevated as much as possible to avoid inflammation and pain.
- Not putting weight on the foot until after the second week of recovery.
- Quitting smoking to prevent nicotine from negatively affecting healing.
- Attending all scheduled post-operative appointments with the surgeon.
- Contacting the surgeon immediately if there are any unusual situations such as excessive bleeding, excessive inflammation, pain, redness, itching, etc.
- Eating a healthy and balanced diet.
- Applying ice to the foot during the first few days to reduce pain and inflammation.
- Taking vitamin C supplements a few weeks before and after surgery.
Non-surgical treatments for Haglund's deformity
Before performing surgery for Haglund’s deformity, patients are recommended to try one or several non-surgical or conservative treatments. Many patients improve with conservative treatments, which include:
Medication: Non-steroidal anti-inflammatory drugs (NSAIDs) may be used to reduce inflammation and pain. Topical pain relievers and corticosteroid injections can also be applied to the affected area. However, long-term use of medication may have unwanted side effects.
Ice compresses: Applying ice compresses can help reduce swelling. The ice should be wrapped in a cloth or towel before being applied to the skin for 20 minutes at a time, as needed.
Shoe inserts: Heel lifts can be placed inside shoes, particularly for patients with flat or high arches. These can help reduce pressure on the heel. Heel pads can also be used to cushion the heel and reduce irritation.
Exercise: Stretching exercises can help alleviate tension on the Achilles tendon. Running on hard surfaces or uphill should be avoided.
Shoe modification: Shoes that apply excessive pressure on the heel should be avoided, as they can worsen Haglund’s deformity. Soft-soled or heel-less shoes can help alleviate pain and swelling.
Immobilization: Some patients use immobilization therapy with a cast to reduce symptoms.
Physical therapy: Ultrasound therapy can help reduce inflammation and pain in some cases. Physical therapy exercises can also help strengthen the muscles and improve the range of motion.
It is important to note that these conservative treatments may reduce inflammation of the bursa, but will not remove the bony protrusion. If these treatments do not show improvement, surgery for Haglund’s deformity may be necessary.
Frequently Asked Questions
It is important to follow the instructions given by your surgeon during the recovery period after surgery for Haglund’s deformity. During the first 10 days, the foot should be kept elevated and should not be supported on the ground. After this period, if the doctor allows it, the patient can start to support the foot with the use of a special boot provided by the clinic. It is essential to attend all scheduled post-operative appointments with the surgeon and to report any abnormal symptoms such as excessive bleeding, severe pain, redness or itching. Following a healthy and balanced diet, taking vitamin C supplements and applying ice to the foot can also help with the recovery process.
The patient must arrive at the clinic at the time they are scheduled. Legal procedures will be carried out before they are taken to the operating room. The patient will then change into a gown provided by the hospital. The doctor will instruct them to lie down on the operating table in the appropriate position. Anesthesia, either general or local, will be administered as planned. The surgery will not take more than 60 minutes. After the surgery, the patient’s foot will be immobilized and covered with a cast. The patient may also be given an injection to alleviate pain before they return home.
Some physical conditions or health issues can be risk factors for Haglund’s deformity, including:
- Wearing tight-fitting shoes that put pressure on the back of the heel.
- Frequently running on hard surfaces.
- Having an injury or trauma to the ankle joint.
- Having a heel deformity.
- Having an Achilles tendon strain or tear.
- Having flat feet.
- Having a genetic predisposition.
- Being overweight or obese.
- Advancing in age.
The doctor or specialist will perform the necessary tests to determine if the deformity is related to Haglund’s syndrome. During the initial medical examination, the appearance and mobility of the foot will be evaluated. An important characteristic to look for in the diagnosis is the visible protrusion or bump on the back of the heel.
To complete the diagnosis, the doctor may take one or several x-rays. The x-ray, especially in the lateral position of the foot, will show a pronounced bony protrusion or growth in the heel area. The imaging test should also show any calcifications in the Achilles tendon that are causing irritation. Additionally, ultrasound and MRI tests can be done to help determine the state of soft tissues such as tendons, muscles, and bursas. This is where bursitis, or inflammation of the bursa, can be confirmed.
Another test for the diagnosis of Haglund’s deformity is determining the Fowler-Philip angle. This is the angle formed between the lower heel bone and the posterior surface of the heel bone. If the angle measures more than 75 degrees, it indicates the presence of Haglund’s deformity. The larger the angle, the more advanced the stage of the deformity.
The doctor or specialist will perform the necessary tests to determine if the deformity is related to Haglund’s syndrome. During the initial medical examination, the appearance and mobility of the foot will be evaluated. An important characteristic to look for in the diagnosis is the visible protrusion or bump on the back of the heel.
To complete the diagnosis, the doctor may take one or several x-rays. The x-ray, especially in the lateral position of the foot, will show a pronounced bony protrusion or growth in the heel area. The imaging test should also show any calcifications in the Achilles tendon that are causing irritation. Additionally, ultrasound and MRI tests can be done to help determine the state of soft tissues such as tendons, muscles, and bursas. This is where bursitis, or inflammation of the bursa, can be confirmed.
Another test for the diagnosis of Haglund’s deformity is determining the Fowler-Philip angle. This is the angle formed between the lower heel bone and the posterior surface of the heel bone. If the angle measures more than 75 degrees, it indicates the presence of Haglund’s deformity. The larger the angle, the more advanced the stage of the deformity.
Most patients will go home on the same day as their surgery, once the effects of general anesthesia have worn off. However, it’s recommended to wait for about 10-12 hours before doing so, as a drain may be left in place to prevent hematoma formation. Only patients with other significant medical issues will be required to stay overnight for observation of their post-surgery recovery. If all parameters are good the next morning, the patient will be able to return home.
After surgery, patients will leave with a cast or bivalve splint covering the lower leg. This dressing should be kept clean and dry until the tenth day, when it will be removed to allow for the removal of surgical stitches. Patients should not move or remove the dressing themselves.
After 2 weeks following surgery, patients can return to wearing normal shoes and can begin to engage in light activities such as walking. Daily walking, without over-stressing the foot, will help to strengthen the muscles and tendons. Gradually increasing distances is recommended. Running should not be resumed until at least 3 months have passed, while more intense sports activities should be avoided for 9 months.
A physiotherapist will provide the patient with a detailed rehabilitation program. Some people may become frustrated because they feel they are progressing slowly and have lost the athletic abilities they had before surgery for Haglund’s deformity. However, with consistency and patience, many will be able to achieve the expected level. Regaining full strength and balance can take some time.
The appropriate time to resume driving is from the sixth week of recovery, when normal shoes can be worn again. Before driving freely, we recommend doing some tests:
- Sitting in the driver’s seat and, without turning on the car, testing the pedals several times to ensure that we have enough strength in the feet to react in time during driving.
- Driving slowly around the street of the house, without going far, and on less busy streets.
- If the patient feels good control over the vehicle, they can begin to make short trips, not too far from the starting point.
- Having acquired all the necessary skills, the patient can drive freely.
If the car is an automatic, and the surgery for Haglund’s deformity was performed on the left foot, it is likely that the patient can drive earlier than indicated, after the second week. However, as this may involve some risk, it is better to consult with the doctor. Additionally, it is important to consult with the car insurance company and know the conditions to cover any possible accident
The answer to this frequent question will depend on the type of work that the patient does. For those who have a sedentary or desk job, where the operated foot can be kept elevated, they can return to work after the first 2-3 weeks of recovery. If the job is very active, physical, or strenuous, and involves standing or moving around, the patient will need more recovery time before they can return to work. They probably can start from the third month of recovery.
It is not recommended to fly when the surgery is still recent, as this increases the risk of blood clots forming. Blood clots pose a risk of deep vein thrombosis or DVT, which is extremely dangerous for one’s life. It’s recommended to consult with the surgeon about when is the appropriate time to take a flight, as it also depends on the patient’s recovery rate. Furthermore, it’s important to keep in mind that each airline has its own restrictions regarding flying after surgery. Usually, it’s recommended to take a flight only after the first 10 to 14 days of recovery.
After surgery for Haglund’s deformity, the patient will have to make several postoperative visits to the surgeon. These visits aim to observe the healing of tissues and bone, as well as the rehabilitation of the foot.
Let’s see:
- Day 10 (first postoperative visit):
- The cast and stitches are removed.
- A radiograph is also taken to observe the position of the bone.
- If the surgery was performed without debridement or repair of the Achilles tendon, a heel-elevating boot will be placed. This allows for progressive weight bearing, from 10 to 100% over the next 4 weeks.
- However, when the surgery involves debridement of the tendon, patients must continue without exerting pressure on the foot for the next 4 weeks.
- Those who required extensive repair will need a new cast to immobilize for a longer period.
- The surgeon will recommend keeping the foot elevated as needed.
- Sixth week (second postoperative visit):
- When the surgery for Haglund’s deformity did not involve restoration of the Achilles tendon, at this time the patient will have the boot removed and can start walking.
- If there was tendon treatment, the patient will have to start supporting the foot gradually or using the boot, according to the doctor’s guidance in each case.
- The doctor will prescribe certain activities depending on the progress and clinical history of each patient.
- Third month (third postoperative visit):
- Starting from the third month, another visit to the surgeon is made to check the current conditions of the foot.
- At this time, if health conditions allow, the patient will be formally discharged.
- However, the patient will be instructed to continue with physiotherapy and gradually increase the level of exercise.
- Physiotherapy is key to improving the strength and resistance of the foot and ankle.
- Patients must be patient, as a complete rehabilitation may take between 10 and 12 months. Even inflammation may last between 6 and 8 months. The use of compression stockings is recommended to prevent it.
The Haglund’s deformity, in many cases, appears due to wrong habits that patients maintain for years without realizing it. Now we will give some tips to avoid this deformity:
- Avoid frequent use of high heels, shoes that have hard and pointed tips. It is more advisable to use soft shoes and those that do not have a heel.
- Do not run frequently on hard surfaces, such as avenues or sidewalks.
- Avoid running on surfaces that are uphill, as this forces the Achilles tendon.
- People with a very high arch, should use arch supports within shoes, so that the plantar support is more complete.
- Use orthopedic devices that help maintain good posture in the foot.
- Practice stretching exercises that prevent the Achilles tendon from cramping.
- McGarvey WC, Palumbo RC, Baxter DE, Leibman BD: Insertional Achilles tendinosis: surgical treatment through a central tendon splitting approach. Foot Ankle Int. 2002 Jan;23(1):19-25. DOI: 10.1177/107110070202300104. PMID (PubMed Identifier): 11822688.
- Bunion Surgery Miami. (n.d.). Haglund Deformity Surgery. Retrieved from https://bunionsurgerymiami.com/haglund-deformity-surgery/
Latest Articles

What to Expect After Haglund’s Deformity Surgery
When Haglund’s deformity proves to be resistant to all non-surgical remedies, such as changing footwear, anti-inflammatory drugs, and physiotherapy, surgical
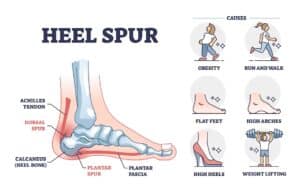
Dorsal Heel Spur Surgery – Procedure, Recovery, and What to Expect
Dorsal heel spur surgery is a procedure that alleviates irritating symptoms caused by heel spurs that develop on the back
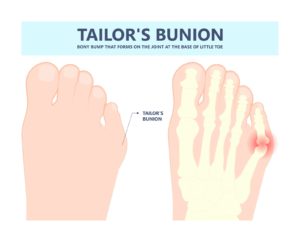
Bunion on the Little Toe: Causes, Symptoms, and Treatment Options
Many individuals struggle with a bunion on the little toe – this condition can cause unpleasant symptoms and interfere with

How to Treat the Bursitis of a Bunion
When there is a bunion, one of the common complications that can occur is bursitis. This condition is an inflammation
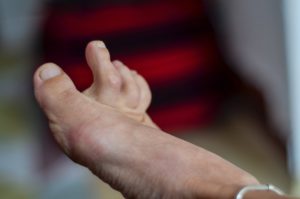
Failed Hammertoe Surgery: Causes, Complications, and Solutions
No matter how experienced a doctor is or how routine the procedure, every surgery poses a certain amount of risk

Floppy Toe After Hammertoe Surgery: Understanding the Phenomenon
Even though hammertoe surgery is a routine, minimally invasive procedure, it still carries a certain amount of risk. One of

Toe Shortening Surgery in Atlanta: A Comprehensive Guide
Foot health is always overlooked until a person starts having difficulties while walking and standing for longer periods of time.

Understanding the Stages of Healing for a Plantar Wart: A Comprehensive Guide
Skin conditions on your feet can be difficult to fully get rid of, which is why it’s so important to

Plantar Wart vs. Callus: How to Differentiate Between the Two
A lot of different skin conditions present themselves in a similar fashion on our feet – rough bumps or patches

Plantar Wart vs. Corn: Understanding the Differences
It’s well-known that plantar warts and foot corns aren’t the same thing – but they still often get confused with

Bone Spur or Bunion: Understanding the Difference
Bone spurs or bunions are different orthopedic issues that can create foot pain and discomfort. Even though they have distinct

Bunion Recovery Week-By-Week Process
Bunion surgery is a highly successful procedure, and most patients recover from it very well and in a short amount
